Save
Much of the day-to-day work of UX design focuses on optimizing manual, paper-based processes through the use of technology. Consider Amazon’s origins, for example. Buying a book from a catalog has been around since 1498 when Aldus Manutius published a catalog of the books he printed. Almost 500 years later, Amazon put their catalog online and created a virtual, online experience for people to buy books.
In Amazon’s early years, this focus led to innovative steps in traditional transaction-based human–computer interaction (HCI). With transaction-based HCI, the user gives a command (search for a book) and the system responds (a list of books). Over time Amazon has introduced a user experience in which the system uses analytics with customer input and actions to identify and recommend potentially interesting books and products. This experience becomes more than simply a sales ally; it is a synergy between Amazon and the customer — an effective partnership in which the outcome produced is greater than sum of the individual efforts.
Human–Computer Synergy
Just as Amazon replaced the printed catalog with an online catalog, healthcare systems have begun to replace mountains of patient records with electronic health records. Unfortunately, many of these systems were developed with minimal UX design considerations and provide primitive transaction-based HCI. This has caused new challenges for practitioners who are frustrated with the way technology impedes their workflow. [1]
We recently worked on a project that focused on the replacement of a medical case management system. Early in our user research we used the System Usability Scale (SUS) to evaluate the existing system. [2] The SUS score of that system was 44.5 out of possible 100 (the average score is 68). The system was so poorly designed that during one user interview a nurse began to cry as she described the various tasks she was required to complete in order to track patients and document her interactions with them.
As the outdated system was slowly replaced with a new system that increasingly incorporated data analytics and artificial intelligence, the SUS scores improved as shown in Figure 1. The synergistic use of AI and analytics led to the development of a richer experience, and the SUS scores improved by more than 100%, jumping to 93.
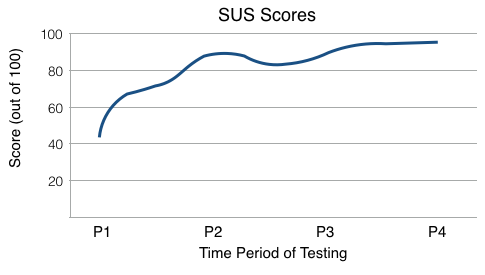
Figure 1: SUS Scores over time
UX designers typically focus on making user interfaces easy for entering, finding, and presenting information. As work domains increase in complexity, workers’ productive capacity must expand beyond their individual capacity, which means they will have to rely more and more on a cooperative relationship with a computer system that has different and complementary skills. The outcome of this relationship, or partnership, will be greater than the simple sum of the human or computer individually — i.e., it will be a human–computer synergy.
A good example of human–computer synergy occurred in 2005 when a team composed of two amateur chess players using three off-the-shelf computers won the Freestyle Chess Tournament. They were opposed by chess grandmasters who were supported by supercomputers, and yet they were able to win by collaborating more quickly and efficiently with the machines. As grandmaster Garry Kasparov explained it: “Weak human + machine + better process was superior to a strong computer alone and, more remarkably, superior to a strong human + machine + inferior process.” [3]
In order to identify hidden opportunities for human–computer synergies in our medical case management system, we added a set of machine-focused questions to our traditional user research questions (see Figure 2). These questions were posed to the software engineering and data analytics teams rather than the users, because the engineers had insight into the potential integrations.

Figure 2: Example integration questions
Their answers to the additional questions guided us to include features in our medical case management system that met the user’s strategic goals along with their tactical goals. For example, we investigated the nursing task of reviewing a patient’s case every 90 days, the goal of which is to review the patient’s progress and encourage them to follow a plan of care. A large number of nurses complained about how time-consuming it could be to locate patients in order to review the case with them, since many patients frequently moved or changed phone numbers.
Rather than simply providing a list of all of the known patient addresses and phone numbers (i.e., a transaction-based approach), data analytics and artificial intelligence algorithms were used to suggest possible friends or family members with whom a patient may be living (i.e., a synergistic approach). This feature delighted the users and it received a SUS score above 90.
Three Types of Human–Computer Synergy
There are many different types of human–computer synergy, but for the sake of illustrating the concept generally we’ll focus on three types: information recall, task management support, and assistance in situation awareness.
Recognition is Easy; Recall is Hard
In Designing with the Mind in Mind, Jeff Johnson illustrates how the human mind is wired such that “recognition is easy; recall is hard.” [4] This was a key consideration throughout our redesign of the medical case management system, and particularly as regarded medication management. As one nurse put it when answering a question about managing medication conflicts: “Common medications are common.” Nurses must be familiar with the uses and side effects of different medications, and apply that knowledge quickly in everyday decisions. There are thousands of medications, some of which are have uncommon interactions or uncommon counterindications, and many of which are infrequently prescribed, and nurses must be able to quickly understand the implications, side effects, and potential conflicts with other medications. Even for the most experienced nurses, this domain can be dangerously error-prone, particularly with complex cases and when medical staff are rushed or overworked.
Fortunately, an effective partnership between nurses and their information systems can radically decrease risks, improve outcomes, and also improve the quality of the nurse’s experience of their work. We focused designing ways for the case management system to deliver the right information to nurses at the right time and with great accuracy, and thus shift much of the challenge from recall to recognition. This led us to introduce simple, recognition-oriented features such as the ability to search phonetically in addition to alphabetically, as well as more complex features that teed up key information about a medication and its relationship to the others in the patient’s active medication list. This human–machine partnership included the machine in the medication review process, and supported the nurse’s clinical workflow. It aided the human recall task, and facilitated faster recognition.
Task Management
As part of the case file, nurses maintained a task list that included items such as direct existing communication, medication updates, and annual health reviews. The nurses described the original system as time-consuming, highly manual, and often redundant. They showed us many workflows that were designed with more concern to system constraints, rather than the patient’s or nurse’s needs. For example, the same patient identification numbers had to be entered into the system in multiple places in order to support a nightly batch process.
A redesigned technical system could of course eliminate those needless burdens, but one of the interesting design questions was: to what degree should the system replace vs. support human intervention? Contrary to what most designs might assume, it is important to the nurses that they do the task management themselves; they believe that their world is too dynamic for a machine to keep up. This is very similar to the findings of a 2008 DARPA-sponsored project whose goal was to develop a system that would coordinate and update military mission plans as the mission unfolded. The interesting result of that project was that a team of human schedulers collaborated to achieve better results than two competing automated systems. One of the designers noted: “The most interesting result of the evaluation is that it is so difficult to outscore humans in a complex planning and scheduling problem.” [5] This suggests that the best use of technology is to support and facilitate human planning, rather than attempting to replace it.
Situation Awareness
In 2016, Johns Hopkins University estimated that over 251,000 people die each year due to medical error. This was the third leading cause of death in the US (behind heart disease and cancer). [6] Inadequate situation awareness [7] has been identified as one of the primary factors in accidents attributed to human error, and situation awareness is especially important in work domains (e.g., healthcare) where the information flow can be quite high and poor decisions may lead to serious consequences. [8]
For example, in 2005 Elaine Bromiley was booked for endoscopic sinus surgery and a septoplasty, which are relatively routine and low-risk procedures. But before the surgery began, her anesthesiologist had difficulty intubating her, which caused her oxygen flow to be cut off. In order to recover her dropping oxygen levels, he attempted to ventilate her lungs with pure oxygen. When this did not work, he fixated on the intubation process rather than identifying the situation known as “can’t intubate, can’t ventilate.” The anesthesiologist’s lack of situation awareness was determined to be a contributing factor in Elaine’s death. [9] A synergistic, partner technology system that was monitoring the same vital signs as the anesthesiologist might have been able to pull the anesthesiologist out of his tunnel vision by urgently presenting an emergency checklist for that type of crisis, and might have recognized the crisis as so severe and urgent that alarms should be automatically sounded to call for help.
While the systems you design may not be critical to life support, any support that technology can provide to the user’s situation awareness will likely increase the usability. As demonstrated in increased SUS scores, our users appreciated improved understanding of a patient’s overall situation through the last known sightings feature, and increased awareness of possible medication conflicts.
Conclusion
Albert Einstein famously noted, “We cannot solve our problems with the same thinking we used when we created them.” Complex domains such as healthcare require a new way of thinking about both the problem and the solution. Sometimes traditional, transaction-based HCI may not be enough. UX designers may want to consider viewing the machine as a partner rather than just a system, and use a synergistic approach to the design of human–computer systems.
References
[1] Miliard, M. (2016) Frustrations Linger around Electronic Health Records and User-Centered Design. Healthcare IT News.
link
[2] Brooke, J. (1996). “SUS: a “quick and dirty” usability scale”. In P. W. Jordan, B. Thomas, B. A. Weerdmeester, & A. L. McClelland. Usability Evaluation in Industry. London: Taylor and Francis.
link
[3] Kasparov, G. (2010) “The Chess Master and the Computer,” The New York Review of Books, February 11.
link
[4] Johnson, Jeff. (2014) Designing with the Mind in Mind. Morgan Kaufmann
[5] Maheswaran, R., Rogers, C. M., Sanchez, R., Szekely, P., Gati, G., Smyth, K., & VanBuskirk, C. (2009). Multi-agent Systems for the Real World. Proceedings of The 8th International Conference on Autonomous Agents and Multiagent Systems. Vol. 2, pp. 1281-1282.
[6] Cha, A. E. (2016) Researchers: Medical Errors now Third Leading Cause of Death in United States. The Washington Post. May 3, 2016.
link
[7] Endsley, Mica R. (1995) “Toward a theory of situation awareness in dynamic systems.” Human Factors: The Journal of the Human Factors and Ergonomics Society 37.1, pp. 32-64.
[8] Hartel, C.E.J., Smith, K., & Prince, C. (1991). Defining Aircrew Coordination: Searching Mishaps for Meaning. Proceedings of the 6th International Symposium on Aviation Psychology.
[9] Fioratou, E., Flin, R., Glavin, R., & Patey, R. (2010) Beyond Monitoring: Distributed Situation Awareness in Anaesthesia. British Journal of Anaesthesia 105 (1), pp. 83-90.
Lisa J Douglas
Innovative UX and Human Factors leader with a fresh perspective. I use my skills and experience to help organizations translate business strategy and user needs into awesome technology. PhD in Human Factors Psychology.
Strategic and tactical experience managing all phases of research and design for complex socio-technical domains including healthcare, legal, and military to understand user / customer needs, innovate product concepts, and drive design decisions. Experience also includes research and budget program management, and theoretical and experimental design and analysis in applied cognition and memory, and perception.
I've successfully developed and managed cross-functional HF/UX teams in B2B and B2C projects. I've worked closely with PM, SMEs, and users, as well as project leads, UX, back- and front-end developers in an agile and systems thinking environment. I have extensive experience in UX research and design. My toolkit comprises all phases of product development including ideation, wireframing, interaction design, prototyping, concept and usability testing, contextual inquiry / interviews, affinity and journey mapping, and survey development.