For years, I have been addressing how UX can move upstream to play a more substantive, strategic role in business. An example of this was my CHI 2007 panel entitled, Moving UX into a position of corporate influence: Whose advice really works? Another example was my Mx 2008 presentation emphasizing the challenges UX personnel face when attempting to move their work upstream.
Related challenges (and warnings) were emphasized more recently by Samantha Starmer and Greg Laugero. Starmer argues:
Given the current power of CX at the C-level, UX practitioners must step up our game, otherwise we will lose progress we have made to be more deeply involved in strategy beyond just performing usability services. We need to act now to be part of the broader CX solution. If we don’t proactively collaborate across divisions and organizational structures, we will be stuck playing in the corner by ourselves. If we don’t figure out how to manage partnerships with other departments in a collaborative, creative, customer focused way, the discipline of UX as we know it is at risk. CX management will take over.
UX design has done a great job in the last decade of redefining (for the better) how we define requirements for products with digital UIs. There is no doubt about this. But this has come at a cost of upward mobility in our organizations. We’re functional players that make tactical work more efficient. We’re not strategic players that help our organizations transform themselves. The closer we look at UIs, the more pigeonholed we’re likely to be.
…stepping up [to strategic challenges] may mean stepping out of our comfort zones. …we can’t go in waving deliverables — our standard bulwark. We have to step out from behind our wireframes and prototypes and think strategically.
However, will such a strategic focus actually satisfy UX personnel who have so often complained of corporate marginalization? Jon Kolko argues that the answer will often be “no” since most are actually interested in doing much more meaningful and socially impactful work than is found in most corporations and consultancies. Consequently, Kolko calls on designers to reject the confines of the short-term focused, marketing-driven corporate world to become social entrepreneurs to get the opportunity to tackle some of the world’s many “wicked problems.”
One of those wicked problems: a U.S. healthcare system declared “broken” by speaker after speaker at Stanford’s Medicine 2.0’11 conference. This has been echoed by many, including Donald Berwick M.D., who oversaw Medicare and Medicaid until this past December:
Health care is broken… We have set up a delivery system that is fragmented, unsafe, not patient-centered, full of waste, and unreliable. Despite the best efforts of the workforce, we built it wrong. It isn’t built for modern times.
UX personnel have worked in the world of healthcare at the level of the UI for years. Yet, many medical UIs haven’t benefited from the input of UX personnel and most of the thousands of healthcare apps available today have been designed for the wrong people, and it is not clear how many of them really work. Even if more apps were well designed and did work, would that fix what is broken with healthcare?
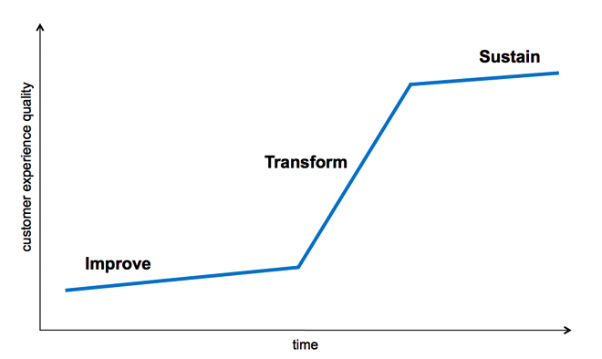
To put the problem in UX/CX terms, what is really needed is transformation of the healthcare customer experience—i.e., what is often referred to as the “patient” experience. And what’s truly needed isn’t just improvement, but is transformation, as captured by this graph from Forrester Research’s Kerry Bodine.
Can UX personnel contribute to this transformation? Laugero doesn’t think so—not so long as UX personnel have an excessive UI focus.
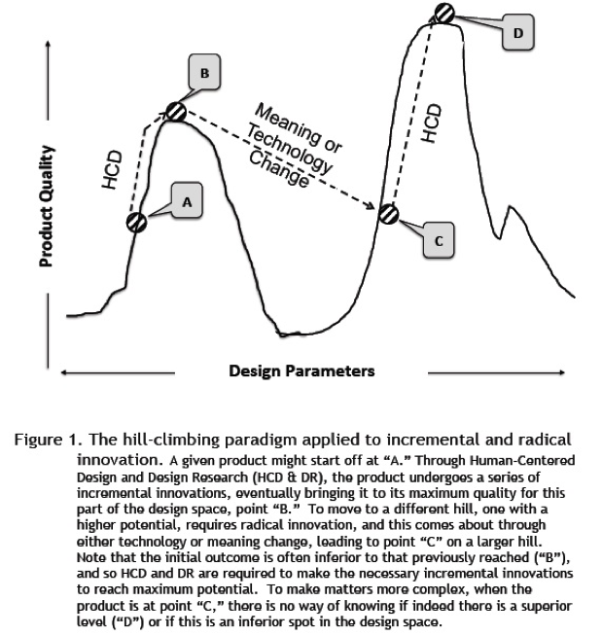
In a recent paper, Don Norman and Roberto Verganti argue that human-centered design as practiced by most UX professionals can contribute to only incremental innovation—”improvements” to existing products or services. Radical innovation (a.k.a. “transformation”), on the other hand (see accompanying figure), requires technology or meaning change, the second of which can be achieved only via the comprehension and change of the dynamics—often subtle and unspoken—of socio-cultural models at play. According to Norman and Verganti as well as Jon Kolko, the design research that is often a part of the human-centered design process typically doesn’t reveal such dynamics. According to Norman and Verganti, the focus of design research is usually not on such meanings; according to Kolko, the amount of time typically allotted to design research is too short to allow for their discovery.
Kolko argues that participatory design—the practice of designing with rather than designing for—can provide the time via which adequate empathy can be built to reveal the deep, tacit, knowledge-holding “critical truths and assumptions about behavior, policies, norms, and values.”
But there are sometimes other sources of this information as well. In the field of healthcare, I’ve found TED talks to be a great source, and I’ve written about them (and other sources) in In need of transformation: the patient experience. For example, four powerful TED talks disclose the great extent to which medicine is conducted in a culture of physician superiority (USC’s Dave Logan), anti-creativity (Jay Parkinson M.D.), denial of mistakes (Brian Goldman M.D.), and treatment of diseases rather than of people (Abraham Verghese M.D.).
Some of these cultural characteristics are reflected subtly in the language of today’s healthcare system, as pointed out by a group of designers led by Hugh Dubberly:
We call individuals “patients.” We call physicians healthcare “professionals” (HCPs). Professionals “care for” patients—by observing symptoms, diagnosing diseases, and proposing therapies. Their proposals are not just suggestions; they are prescriptions or literally “physician orders.” Patients who don’t take their medicine are not “in compliance.”
In the relationship between HCPs and patients, HCPs dominate. HCPs do whatever is necessary, with patients playing a relatively passive role. In some ways, the system reduces patients to the status of children—simply receiving treatment.
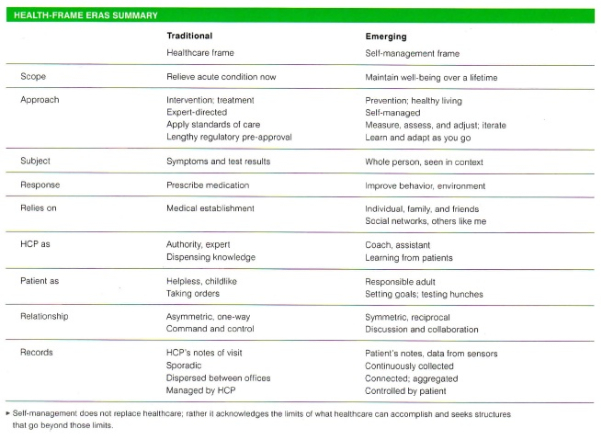
Dubberly et al., focusing on the level of meaning as described by Norman and Verganti, describe an alternative healthcare model of self-management that is contrasted with today’s model in the chart below. This alternative model is consistent with a growing “e-patient” movement supported by the new Society for Participatory Medicine, a movement “in which networked patients shift from being mere passengers to responsible drivers of their health, and in which providers encourage and value them as full partners.”
Much more work along these lines is needed. As stated by rebel Jay Parkinson M.D.:
Going to the doctor, having routine surgery, buying bulk medications online—all could be radically reinvented with the application of one type of medicine: designed disruptive innovation. Combining the principles of disruptive innovation with design thinking is exactly what health care in America needs. We need to disrupt the current business model of health-care delivery. And we need these disruptions to be designed experiences that are consumer-focused.
Recently, Valerie Casey issued a call to action in a short article entitled, Healthcare Innovation: Time for Design(ers). She encourages designers to respond to four innovation challenges issued by large pharma companies and healthcare organizations.
In my view, UX designers can do more. Learn about the problematic cultural characteristics that dominate healthcare and that need to change. Alter how you do design research. Don’t limit yourself to incremental innovation or work that’s narrowly focused on UIs. Question the advisability of doing projects that, in essence, only amount to putting lipstick on the very large healthcare pig. Escape your comfort zone in order to have the kind of impact on the world that you desire.
If only it were a matter of the following:
Indeed, designers need to care.